Spider veins, or telangiectasias, are small, damaged, superficial and visible blood vessels under your skin. They appear like spider webs or tree branches. Telangiectasias are also known as thread veins, venous flares, sunburst veins, stellate veins, and hyphen webs. In fact, they are not veins but the smallest part of our circulatory system: capillaries. The term veins is easier to use and understand.
Spider veins can appear anywhere on the skin but most commonly occur on the legs and face. They can originate from arteries, veins, or both. Telangiectasias can present as blue and purple, pink and red, raised, or flat webs.
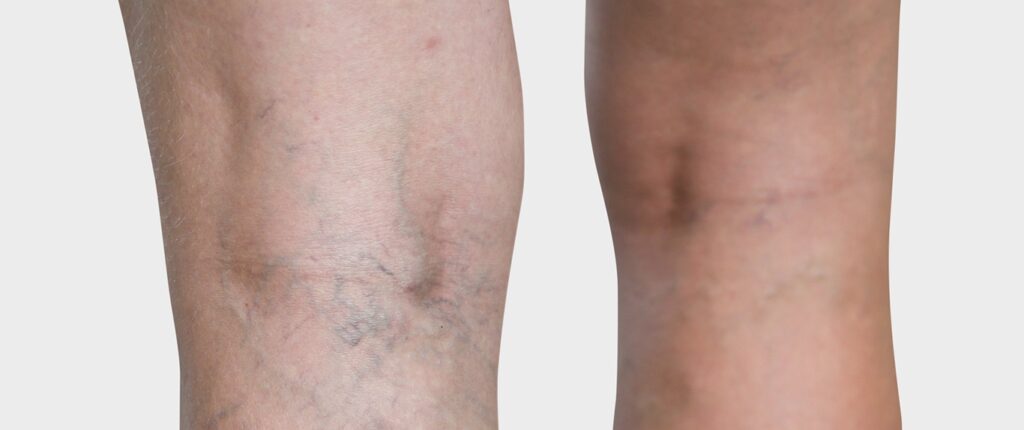
Various studies concluded that almost every adult in the course of their lifetime will develop some form of spider veins. The typical age of presentation is between 30 and 50. In the US, the prevalence is 80% of men and 85% of women.
Causes
The exact mechanism of how spider veins develop is not known. One of the theories is the valvular incompetence of leg veins. The disease is called chronic venous insufficiency (CVI). When vein valves are not working, the blood pools in veins and small vessels and makes them damaged and visible. Against this theory is the fact that only 22.9% of people with spider veins have venous insufficiency.
Risk factors
- Sex: Women are more prone to developing spider veins than men.
- Weight: Obesity (BMI >30)
- Pregnancies
- Use of topical steroids
- Use of hormones for birth control and hormone therapy for menopause symptoms
- Positive family history
- Prolonged sitting or standing
- Low-fiber diet
- Smoking
- Local trauma or thromboembolism
Signs and symptoms
Generally, spider veins are usually an aesthetic problem. If spider veins do not coexist with CVI, most patients are symptomatic. However, a small group of people can complain of burning sensation, itching, cramps, leg pain, and leg fatigue.
Diagnosis and treatment
The diagnosis of spider veins is clinical. However, if there is a suspicion of CVI, tests could be done: duplex ultrasound, contrast venography and magnetic resonance venography. Spider veins can be an early sign of CVI.
Although spider veins are harmless and asymptomatic, people want to remove them generally for cosmetic purposes. The treatment options include sclerotherapy, intense pulsed light (IPL) therapy, thermocoagulation, and microphlebectomy. The choice of treatment depends on individual patient factors.
Sclerotherapy
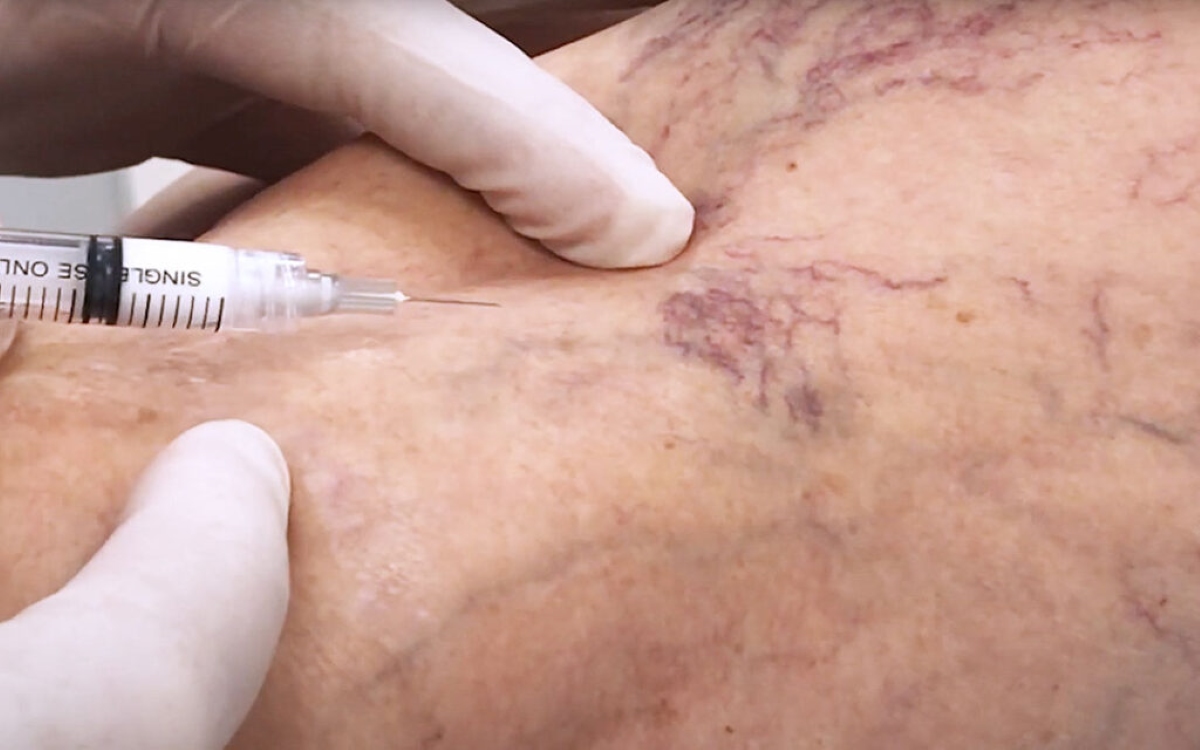
Sclerotherapy is the first-line treatment of telangiectasias on legs. The rate of improvement in patients is 50-70%. The purpose of this method is to obliterate spider veins. With fine-tip needle sclerosing agents, are injected into the vessels under ultrasound navigation. Sometimes you need to undergo more than one procedure to fully get rid of spider veins.
Laser Treatment and Intense Pulsed Light Treatment
Laser treatment and IPL treatment are noninvasive methods for curing telangiectasias. The essence of these methods is the absorption of laser by the vessels and further clot formation and obliteration. These methods are suitable for patients that have spider veins on their face, have an allergy to sclerosing agents, and have needle phobia. Various types of lasers are used for treating spider veins: argon laser, pulsed dye laser, Nd:YAG laser, etc.
Microphlebectomy
Microphlebectomy implicates the extraction of damaged veins through tiny skin incisions or needle punctures. This technique minimizes the risk of adverse events associated with the other procedures: scarring, skin necrosis, and residual hyperpigmentation.
Thermocoagulation
The impact of thermocoagulation on vessels is similar to laser therapy. But instead of laser, the radiofrequency pulse is derived into vessels with a fine tip needle. Created heat destroys the inner layer of spider veins and leads to vein obliteration.
Prevention
As already mentioned, there are modifiable risk factors that can be managed for spider vein prevention. Here are some tips:
- Avoid prolonged standing or sitting. Try to change the position from sitting to standing every 30 minutes.
- Flex your feet and ankles. If you are in the same position for a long time, flex your ankles up and down.
- Keep a healthy body weight.
- Avoid tight clothing.
- Exercise regularly.
- Eat a heart-healthy diet.
- Wear compression stockings. Note that compression therapy should be used only by healthcare professionals’ indication.
When to refer to a specialist?
- There are signs of blood clots: spider veins appear swollen and red or feel warm and tender.
- There is a rash or sores on your skin.
- Skin color has changed.
- You have symptoms that interfere with your daily life.
Prognosis and complications
Summing up, spider veins are simply an aesthetic issue and couldn’t lead to health impairment. Yet, if spider veins coexist with CVI, the complications could be very severe: sores, skin ulcers, and thromboembolism. If you notice spider veins, talk to a healthcare provider to exclude CVI.






