Gastroesophageal reflux, also called “acid reflux,” is a condition when stomach contents and acid flow back to the esophagus, causing unpleasant sensations.
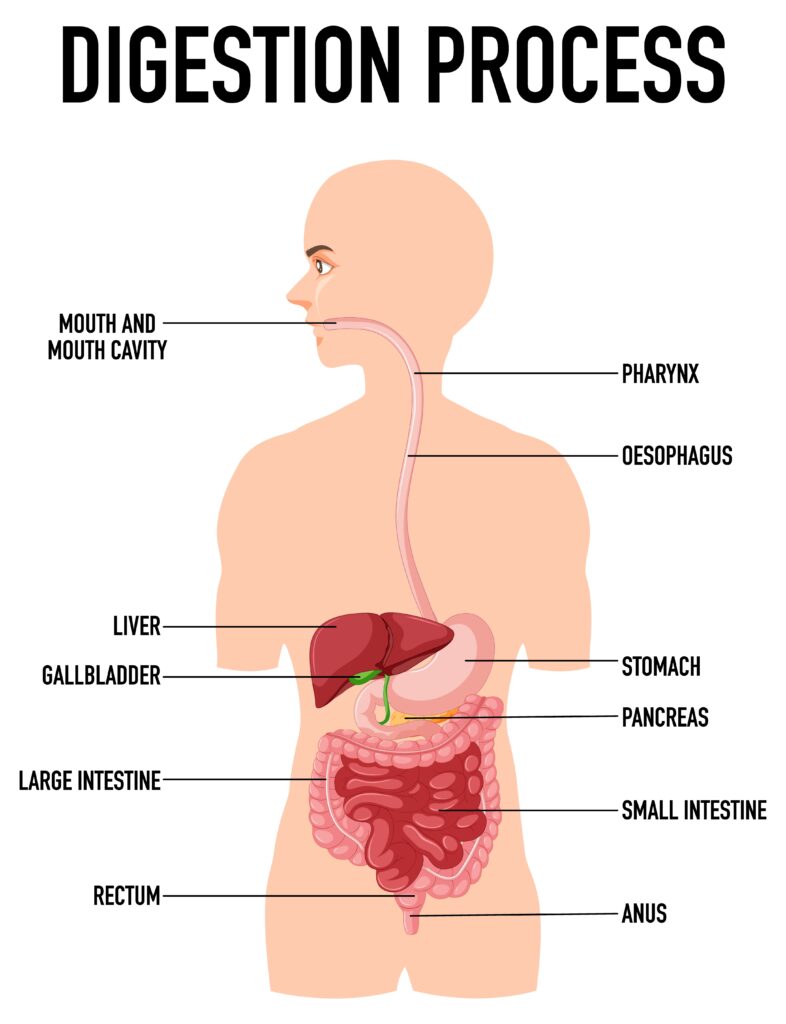
Human digestion starts from the mouth, where food is processed and moved to the esophagus. The esophagus is a tube-like organ with a muscular layer. The latter contracts and drives food to the stomach. Between the esophagus and stomach, there is a circular ring of muscles called the lower esophageal sphincter (LES). At the start of digestion, the LES relaxes to allow food to reach the stomach. Afterward, it contracts to prevent backward movement of stomach content to the esophagus. The LES is surrounded and augmented by a diaphragm; this tandem is called an antireflux barrier.
Sometimes the antireflux barrier fails, and stomach contents drive back to the esophagus (gastroesophageal reflux). It can happen occasionally to everyone, generally after heavy meals. Usually these refluxes are short and rarely cause bothersome symptoms. However, if reflux occurs frequently and causes injury to the esophagus, it’s considered gastroesophageal reflux disease (GERD).
Risk factors
Certain known risk factors increase the likelihood of having GERD.
- Hiatus hernia—In case of this condition, the part of the stomach is pushed up through the diaphragm, and the LES is moved to the chest cavity instead of the abdomen. As a result, the diaphragm fails to augment the function of the LES.
- Obesity—Obese and overweight people have a higher risk of developing GERD and hiatal hernia, related to people with normal BMI.
- Pregnancy— GERD is temporary and usually resolves after delivery.
- Lifestyle factors— Some foods augment GERD: fatty foods, peppermint, and chocolate. Caffeine , alcohol, and tobacco are also related to high rates of GERD.
- Connective tissue disorders —e.g., scleroderma
- Medications—e.g., aspirin
Symptoms
- Heartburn: burning sensation in the chest and throat. Heartburn usually happens after a meal and gets worse while lying.
- Regurgitations: stomach acid and food backwash into your mouth or throat.
The less common symptoms are:
- Stomach pain
- Chest pain
- Difficulty swallowing or pain during swallowing
- Persistent laryngitis (inflammation of vocal cords)/hoarseness
- Persistent sore throat and cough
- New or worsening asthma
- Globus sensation in throat
- Nausea and/or vomiting
When to see a doctor
Seek immediate medical care if you have new chest pain, especially combined with shortness of breath and/or pain radiation to the arm or jaw. These could be signs of a heart attack.
Make an appointment with a healthcare professional if you:
- Have difficulty or pain with swallowing.
- Have no appetite or lose weight without trying.
- Have chest pain.
- Feel like you are choking.
- Have signs of bleeding in the gastrointestinal tract, such as blood in your vomit or dark-colored vomit that looks like coffee grounds or black tarry stools.
- Have persistent vomiting.
- Have new stomach pain and are 60 or older.
- Take nonprescription heartburn medicines more than twice a week.
Diagnosis
Usually, the diagnosis of GERD is made based on “classic” symptoms: heartburn and regurgitation. After disease history and clinical evaluation, your healthcare provider will likely suggest a trial of GERD medication. If symptoms improve, the diagnosis is confirmed.
It is important to rule out life-threatening diseases with GERD-like symptoms, such as heart attack.
In case of a non-classic disease course or suspicion of another cause of symptoms, additional tests (upper endoscopy, prolonged esophageal pH study, esophageal manometry) may be indicated.
Upper endoscopy
A small flexible tube is passed through your mouth to your stomach. The doctor is able to directly examine your upper GI tract. In severe reflux, esophageal mucosa is inflamed, and ulcers appear. Sometimes tissue samples may be taken (biopsy) to determine the origin and extent of tissue damage.
GERD complications
Generally, with sufficient treatment, serious complications rarely occur. However, severe GERD leads to significant complications.
- Erosive esophagitis—Esophageal lining is inflamed and damaged. This leads to esophageal lining erosions and ulcers that can bleed.
- Esophageal stricture—Damage from acid leads to scar formation and narrowing of the esophageal lumen.
- Barret’s esophagus—As a result of long-lasting GERD, normal esophageal cells are replaced by intestinal cells. These changes increase the risk of esophageal cancer.
- Respiratory tract problems—Inflammation of vocal cords, sore throat, hoarse voice, pneumonia, or asthma are rare complications of GERD.
- Dental enamel damage
Treatment
Certain lifestyle and dietary changes can diminish or even relieve the symptoms. If your symptoms are severe, seek professional help, yet for milder symptoms, these tips are recommended:
- Losing weight (if you are overweight or obese).
- Raising the head of the bed 6-8 inches (15-20 cm).
- Sleep on your left side.
- Avoid trigger foods (caffeine, chocolate, peppermint, alcohol, fatty foods).
- Quitting smoking.
- Avoiding late meals.
- Wearing loose, comfortable clothing.
Pharmacological treatment
For mild symptoms:
- Antacids/alginates (Tums, Maalox): these medications neutralize stomach acid. The effect is fast but short-term; it lasts 30-60 minutes.
- Histamine receptor antagonists: these drugs reduce gastric acid production. They are more effective, and the effect lasts longer, but they are not suitable for moderate and severe GERD treatment.
For moderate or severe symptoms:
- Proton pump inhibitors (Dexilant, Nexium, Prevacid) reduce gastric acid production and are effective for moderate and severe GERD treatment.
- Potassium competitive acid blockers (Voquenza) are a new class of drugs that effectively reduce gastric acid production.
Rarely, if symptoms are not controlled with medications, “antireflux” surgery is done.
Sources:
UpToDate
Medscape
MayoClinic







